
The key symptom of sacroiliac joint (SIJ) dysfunction is pain. The sacrum is the tailbone and it connects to the ileum, one of the bones of the pelvis, by ligaments and tendons. Most reports describe patients have pain in one or both buttocks near, or on the posterior superior iliac spine (PSIS). However, pain radiating to the hip, posterior thigh, or even calf has also been described.
Patients explain that pain especially worsens when they have been sitting for long periods or when they perform twisting or rotation movements. They also report:
• Pain quality: The pain is described as a dull ache or sharp, stabbing, or knife like
• Pain distribution: Buttocks, back of thigh, and upper back; can involve one or both sides
• Pain that is worse in the morning (morning stiffness) and resolves with exercise
• Limb lengths may not be equal
• Motion restriction with rotation of the hips
• Pain with touching the area over the sacrum-tailbone
Causes of Sacroiliac Joint Dysfunction
Many patients report that their pain began spontaneously, whereas others
(around 58%) can remember a specific event like trauma. Other factors, such as smoking, poor physical condition, lifting, and obesity, may be contributory, including a family history. Pregnancy is also associated with SIJ dysfunction.
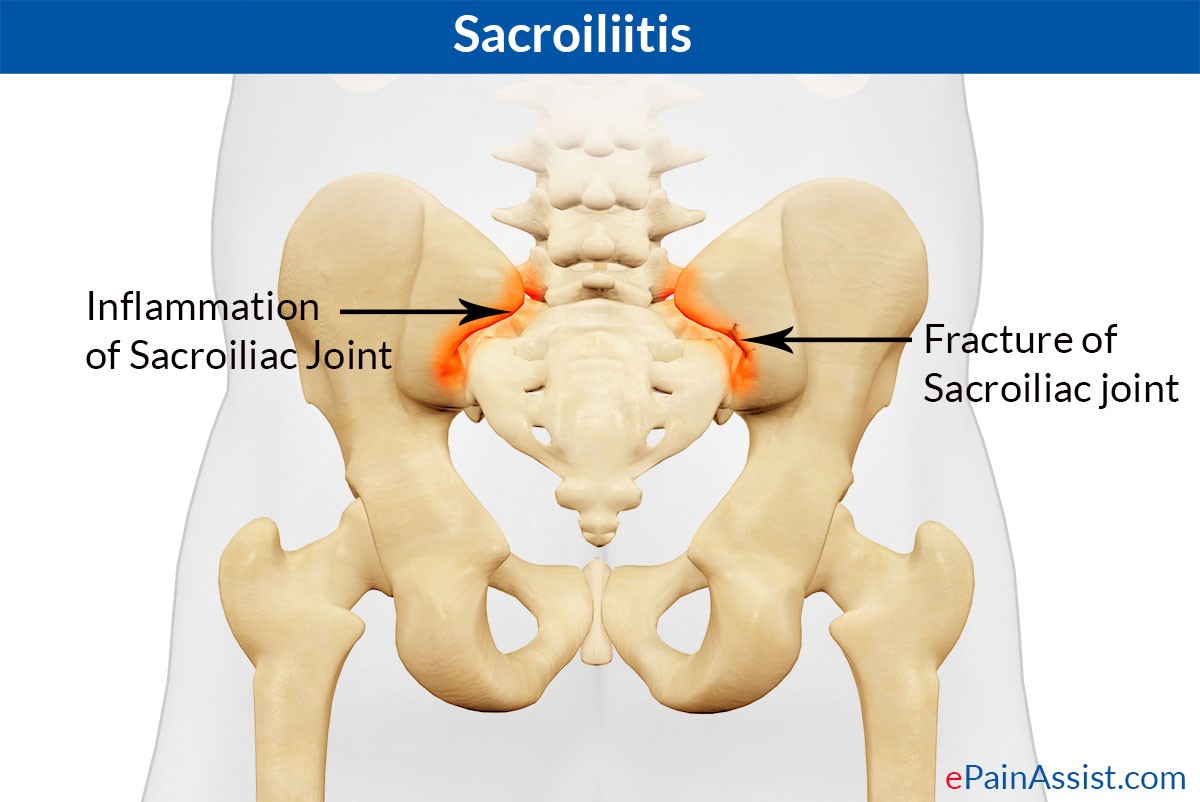
CONDITIONS ASSOCIATED WITH SACROILIAC JOINT PAIN
• Adjacent segment disease (prior spine fusion)
• Ankylosing spondylitis
• Degenerative osteoarthritis
• Degenerative sacroiliitis
• Infection and inflammation
• Leg length discrepancy
• Ligamentous laxity (pregnancy/post pregnancy)
• Sacral disruption
• Sacroiliac Joint disruption (post trauma)
• Structural pelvic asymmetry
• Trauma
• Tumor
Certain bio-mechanical, muscle length or limb imbalances may predispose a person to sacroiliac dysfunction and pain. This is likely due to altered gait patterns and repetitive stress to the SIJ, such as scoliosis, hip osteoarthritis, and poor quality footwear.
Treatment for SIJ Dysfunction
Medications, joint injections, regenerative therapies and physical therapy are all conservative treatments, but if those fail or pain persists for many years a surgical remedy can be indicated. SIJ Fusion entails fusion of the joint to reduce pain and improve stability, and as a relatively new technique is not widely available.
Experienced surgeons like our German specialist Dr. Thomas Bierstedt and our Thai Specialist Dr. Tayard Buranakarl (surgeon instructor for SIJ Fusion) explain indications are very similar to that of a damaged Lumbar Spine, and surgeons should ensure any lower back issues are usually taken care of first.
SIJ Fusion Study Results: What the numbers tell us
A randomized and controlled clinical trial by Polly et al. found that patients who underwent minimally invasive SIJ fusion with triangular titanium implants achieved greater pain and disability relief at 24-month follow-up than did those who underwent nonsurgical management. Six-month success rates were higher in the surgical group (81.4% vs. 26.1%). Clinically important disability index scores showed improvement at six months occurred in 73.3% of the SIJ fusion group vs. 13.6% of the nonsurgical management group.
Another randomized, controlled study by Sturesson et al. found that in the fusion patients (52 subjects), the mean lower back pain score had improved by 43.3 points at six months, compared with 5.7 points in the conservative treatment group, while the mean disability score had improved by 26 points in the fusion patients, compared with 6 points in the conservative management group.
How is SIJ Fusion Performed?
SIJ fusion surgery is performed while the patient is asleep under general anesthesia. Due to advancements in technology and technique, an SI fusion can be a minimally invasive procedure involving one or two small incisions right above the buttock(s) below the waistline, on either side of the spine. Instead of a lateral approach, this posterior approach minimizes injury to surrounding tissue, such as muscle. A synthetic bone matrix is introduced to help strengthen the fusion, with threaded screws to fixate the bone during this time.
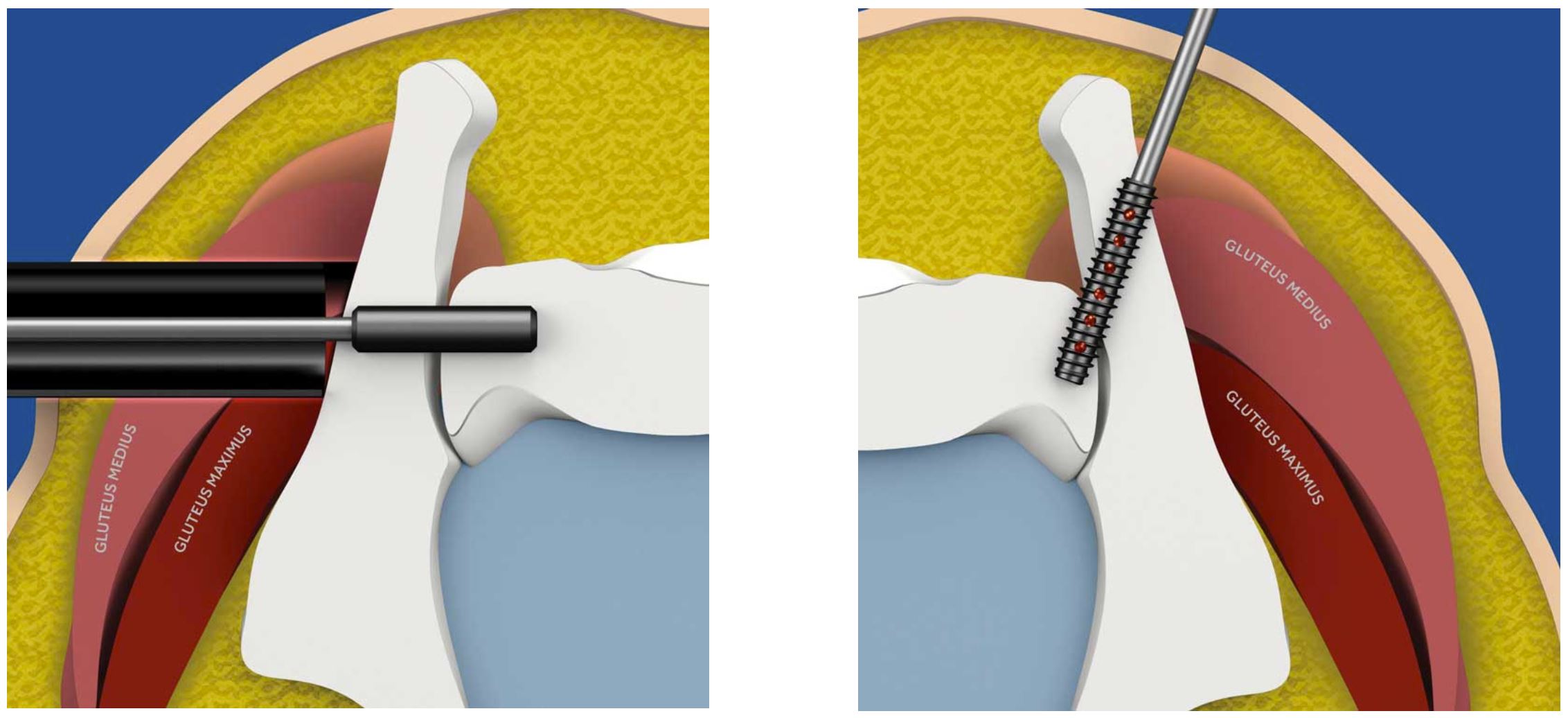
Medical technology company Medtronic has called this their Rialto fusion system. This system uses a posterior approach to the SI joint, which leads to a faster and more complete post-op recovery. Download SIJ Fusion Patient Education Brochure here.
Risks of the Surgery
Compared to an open procedure, this minimally invasive procedure is quick and allows you to go home without a long hospital stay. Some risks are bleeding, haematoma-or collection of blood in the tissue, infection in the skin or deeper tissue, incomplete pain relief, injury to nerves, blood clots in the legs or lungs, and anesthetic complications. Anesthetic complications are rare but are dependent on the overall health of the patient undergoing surgery. Most complications can be managed with medications or rarely a repeat procedure.
Recovery at Home
Postoperatively, you will be shown how to care for your incisions before you return home and your doctor will discuss a program to gradually increase your activity. You may be required to wear a back brace after surgery, and you may be told to avoid repetitive bending, lifting, twisting, and athletic activities while you recover. You may also be cautioned to avoid vibrations, such as those you might experience when driving a car, for a period of time after your surgery.
…………………………………….
References
Polly, D. W., Cher, D. J., Wine, K. D., Whang, P. G., Frank, C. J., Harvey, C. F., Lockstadt, H., Glaser, J. A., Limoni, R. P., Sembrano, J. N., & INSITE Study Group (2015). Randomized Controlled Trial of Minimally Invasive Sacroiliac Joint Fusion Using Triangular Titanium Implants vs. Nonsurgical Management for Sacroiliac Joint Dysfunction: 12-Month Outcomes. Neurosurgery, 77(5), 674–691. https://doi.org/10.1227/NEU.0000000000000988
Sturesson, B., Kools, D., Pflugmacher, R. et al. Six-month outcomes from a randomized controlled trial of minimally invasive SI joint fusion with triangular titanium implants vs. conservative management. Eur Spine J 26, 708–719 (2017). https://doi.org/10.1007/s00586-016-4599-9


